Teacher’s Summary: A student explores the transformative potential of Cognitive Behavioral Therapy (CBT) for addressing mental health issues like depression and anxiety. The essay provides a clear and relatable overview of CBT’s principles, including changing thought patterns and behaviors, and the importance of the therapeutic alliance. By sharing personal experiences and experiments with CBT techniques, the student illustrates how CBT can be applied to everyday challenges such as test anxiety. This thoughtful reflection highlights the practical benefits of CBT for anyone seeking to understand and improve their mental well-being, making it a valuable read for both students and general audiences.
My Journey into the World of CBT: Helping Minds, One Thought at a Time
When my psychology teacher announced we’d be studying Cognitive Behavioral Therapy (CBT) for depression, I thought, “Great, another boring therapy session to learn about.” Boy, was I wrong! As we dove into the topic, I realized this stuff is actually pretty cool and super relevant to our everyday lives.
What’s the Big Deal About Depression?
So, apparently, depression is like the common cold of mental health problems. It’s everywhere! Did you know that 90% of depression cases are handled by regular doctors, not fancy psychiatrists? That blew my mind. It made me think about how many people I know who might be dealing with depression without even realizing it.
Enter CBT: The Superhero of Therapies
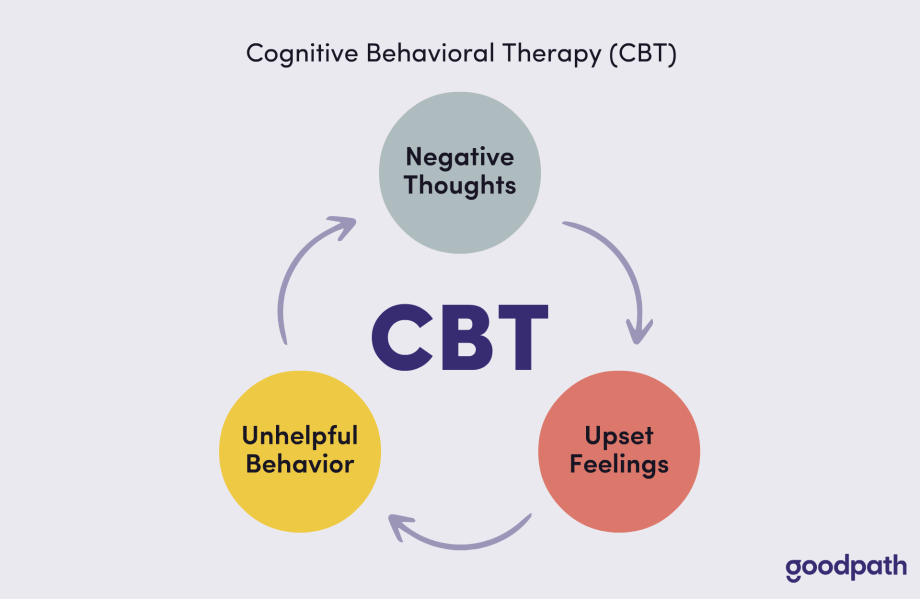
CBT is this awesome therapy that’s all about changing how you think and act to improve how you feel. It’s like giving your brain a makeover. The best part? It’s backed by tons of research, so we know it actually works.
I remember when my friend Sarah was going through a tough time after her parents’ divorce. She started seeing a therapist who used CBT, and it was amazing to see how much it helped her. It made me curious to learn more about how it all works.
The CBT Toolbox: What’s Inside?
- The Therapeutic Alliance: Fancy way of saying the therapist and client need to get along and trust each other. It’s not just about the therapist being smart; they need to be warm and genuinely care about helping.
- Thought Patterns: CBT believes that our problems come from messed-up ways of thinking. Like when I bombed that math test and thought, “I’m just stupid and will never be good at math.” CBT would help me challenge that thought.
- Behavior Patterns: It’s not just about thoughts; it’s also about what we do. CBT looks at how our actions affect our mood and tries to change unhelpful behaviors.
- Self-Help Materials: Therapists often give “homework” to help you practice new skills. It’s like having a personal trainer for your mind!
My CBT Experiment: Tackling Test Anxiety
After learning about CBT, I decided to try it out on my own test anxiety. Here’s what I did:
- Identified Negative Thoughts: “I’m going to fail this test and everyone will think I’m dumb.”
- Challenged Those Thoughts: Is failing one test really going to make everyone think I’m dumb? Probably not.
- Changed My Behavior: Instead of cramming the night before, I started studying a little bit each day.
- Practiced Relaxation: I learned some deep breathing exercises to calm my nerves before tests.
And you know what? It actually helped! I still get nervous, but it’s way more manageable now.
The ABC-E Model: A Cool Way to Understand Your Mind
One of the coolest things I learned about was the ABC-E model. It’s like a roadmap for understanding how our thoughts, feelings, and actions all connect:
- A: Activating Event (what happened)
- B: Beliefs (what you think about it)
- C: Consequences (how you feel and act)
- E: Environment (what’s going on around you)
For example:
- A: Got a C on my English essay
- B: “I’m terrible at writing. I’ll never get into a good college.”
- C: Felt depressed, didn’t want to do my homework
- E: Parents pressuring me about grades, upcoming college applications
Understanding this helped me see how my thoughts were making me feel worse, and how I could change them to feel better.
Why CBT is So Cool (Even if You’re Not Depressed)
The best part about learning CBT is that it’s useful for everyone, not just people with depression. It’s like a Swiss Army knife for your mind. You can use it to:
- Manage stress (hello, exam season!)
- Improve relationships (no more jumping to conclusions about what your friends think)
- Boost self-confidence (bye-bye, negative self-talk)
- Set and achieve goals (by breaking them down into manageable steps)
Conclusion: My New Outlook on Mental Health
Learning about CBT has totally changed how I think about mental health. It’s not just about “fixing” problems; it’s about giving everyone tools to understand their minds better. I’ve started paying more attention to my thoughts and how they affect my mood, and I’ve even shared some of what I’ve learned with my friends.
Who knew that a therapy technique could be so interesting and useful? CBT might not be able to solve all of life’s problems, but it sure gives us a great toolkit to tackle them. Next time someone tells me to “think positive,” I’ll know there’s actually some solid science behind that advice!
Work Cited:
- Beck, A. T. (1976). Cognitive Therapy and the Emotional Disorders. International Universities Press.
- Burns, D. D. (1999). The Feeling Good Handbook. Penguin Books.
- Greenberger, D., & Padesky, C. A. (2015). Mind Over Mood: Change How You Feel by Changing the Way You Think. The Guilford Press.
- Leahy, R. L., & Holland, S. J. (2000). Treatment Plans and Interventions for Depression and Anxiety Disorders. The Guilford Press.
- Cambridge University Press. (2016). Cognitive Behavioral Therapy.